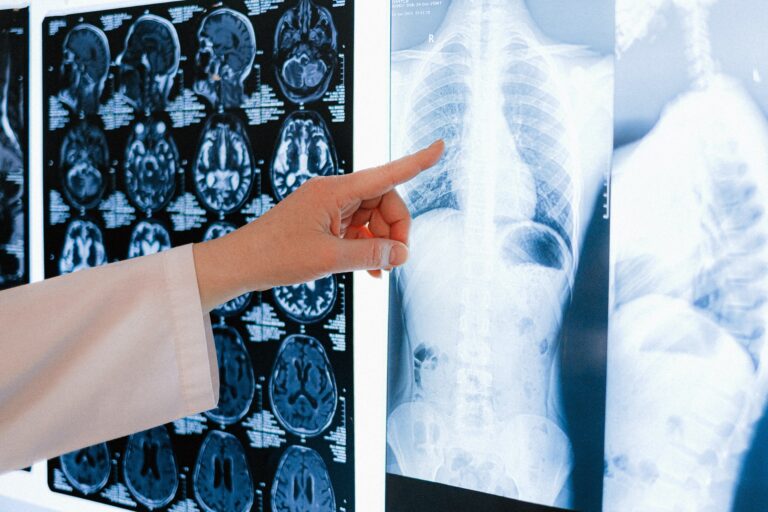
Maddy Smith was diagnosed with Spinal Muscular Atrophy (SMA)—an extremely rare but debilitating genetic disorder—as an infant. SMA is a neuromuscular condition that robs victims of the ability to move, swallow, and sometimes breathe without assistance. Shortly before she turned two, Maddy still lacked the strength to crawl or eat solid foods.
Who Should Decide if Weight-Loss Injections Should be Prescribed for Kids?
The latest statistics from the National Health Institute find about 43 percent of US adults are considered obese. Ten percent of US adults are categorized as severely obese—with BMIs over 40 percent. As alarming as these figures are, childhood and young adult obesity rates aren’t far behind.
More Oversight Won’t Help the US Baby Formula Market
Between September 2021 and February 2022, the Food and Drug Administration received complaints that infants became ill and perished after consuming powdered baby formula. These formulas were eventually traced back to a large manufacturer in Sturgis, Michigan. After a stern warning from the FDA, the plant shut down and issued significant recalls. Other producers quickly followed their lead.
The FDA Should Stay Away from Laboratory Developed Tests
In healthcare, tests are our eyes into the body’s secretive operations. Whether being swabbed for COVID-19, tested for a genetic condition, taken a drug test, or undergoing routine blood work ordered by your doctor, you’ve likely used a laboratory developed test (LDT). About 70 percent of all medical decisions in the US are based on LDT results.
The Pandemic is Over, But Pandemic Policies Are Not
President Biden told us over a year ago that “the pandemic is over.” While the virus is still mutating, the worst is clearly behind us. Recent data compiled by the Centers for Disease Control’s COVID data tracker estimates that COVID-19 causes less than 1 percent of new deaths.
FDA Efforts to Curb Youth Vaping Continue to Come Up Short
Most people associate the Food and Drug Administration with regulating prescription drugs and other medical goods. The agency’s actual regulatory power extends to about 20 percent of all US consumer goods. Some of its authority extends over large portions of the economy—affecting the entire healthcare market and the quality of life for millions of Americans.
The FDA Loosens Blood Donation Restrictions, Finally
For a federal agency tasked and trusted with deciding whether the latest medical goods and procedures should be on the market, the FDA seems hopelessly behind the times. But a recent reversal of a forty-year ban is a step in the right direction.
Recent Attacks on Recreational Marijuana Legalization Are All Smoke
In 2012 Colorado and Washington became the first states to legalize marijuana for recreational use. Minnesota recently became the 23rd. Maryland, New Jersey, and Minnesota are expected to follow soon. When they do, 25 states and Washington DC will allow adults to use a Schedule 1 substance recreationally.
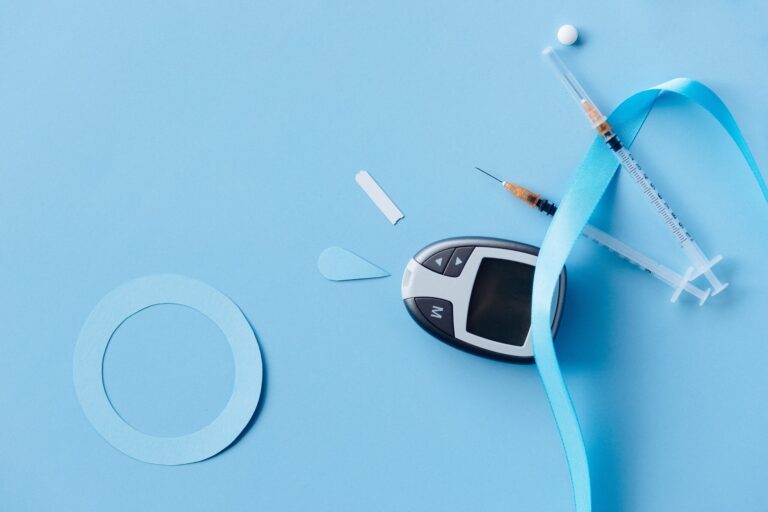
Are Insulin Prices About to Drop? The Devil is in the Details
On March 1st, 2023, Eli Lilly announced in a news release it plans to cap out-of-pocket insulin costs for patients using many of its insulins to $35. These dramatic price cuts aim to make a vital medication for people with diabetes needing it to manage their blood glucose and prolong their lives more affordable. As Eli Lilly Chair and CEO David Rick stated,
FDA’s Rare Positive Move
The Food and Drug Administration is often said to save patients’ lives by only allowing safe and effective products into the US healthcare system. Numerous research articles written over dozens of years strongly indicate it doesn’t—quite the opposite.